What Happens to the Body During Detox? The Medical Side of Recovery
08/18/2025
When people think of detox, they often imagine a quick cleanse or a few rough days of discomfort. But the truth is, medical detox is a complex, sometimes intense process that involves your entire body working to reestablish balance. Whether you’re detoxing from alcohol, opioids, or other substances, understanding the physical experience can make recovery feel a little less mysterious—and a lot more manageable.
Let’s take a closer look at what happens inside your body during detox and why medical support is often crucial for safe and effective healing.
Withdrawal Begins: Your Body Reacts to Absence
Once you stop using a substance your body has grown dependent on, withdrawal symptoms can begin within hours. This happens because your brain and body have adapted to the substance’s presence. Without it, your system becomes chemically imbalanced, causing symptoms like anxiety, sweating, nausea, insomnia, or even seizures, depending on the drug. These reactions aren’t just unpleasant—they can be dangerous. That’s why many people seek professional help through rehab Sydney programs that offer medical supervision and support to ease withdrawal symptoms safely. Medical detox facilities monitor vital signs and can administer medications to reduce risks and keep the body stable.
The Brain Triggers Chemical Shifts

Substance use often hijacks the brain’s reward system, flooding it with dopamine and other feel-good chemicals. During detox, dopamine levels drop sharply, leading to emotional lows, depression, and mood swings. These changes can make it difficult to stay motivated and emotionally steady in the early days of recovery. Over time, the brain begins to regulate its chemistry again. This process takes patience. Medical professionals may prescribe temporary medications or recommend therapies to help the brain adjust and to support emotional health during this vulnerable stage.
The Liver and Kidneys Kick Into Gear
Your liver and kidneys are the body’s primary detox organs, filtering out waste and toxins. When substance use stops, these organs begin working overtime to clear out chemical buildup. In the first few days of detox, this internal cleanup can cause fatigue and dehydration, especially if the person hasn’t been eating or drinking properly. Hydration, nutrition, and medical monitoring are vital here. Medical detox programs often provide IV fluids, supplements, and meals tailored to support organ function and boost energy levels as the body cleans itself from the inside out.
The Heart and Blood Pressure Stabilize
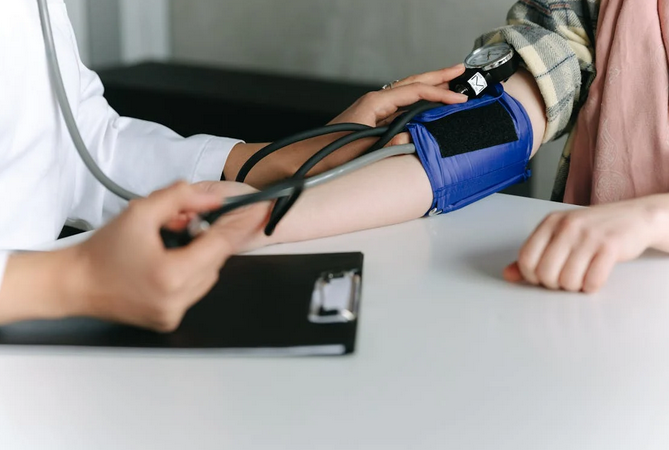
Stimulants, alcohol, and opioids can significantly affect heart rate and blood pressure. As the body detoxes, the cardiovascular system may go through waves of instability—racing heartbeats, palpitations, or even dangerous spikes or drops in blood pressure. That’s why heart monitoring is standard in many medical detox settings. Stabilizing the cardiovascular system is a critical part of early recovery, helping prevent complications and ensuring that the body is strong enough for the next steps of treatment.
Sleep Patterns and Appetite Begin to Normalize
Sleep and appetite are usually disrupted during active substance use. Detox can initially make these issues worse, with people experiencing insomnia, vivid dreams, or a complete lack of appetite. But as the body adjusts, circadian rhythms begin to reset, and hunger signals return. Sleep and proper nutrition are essential for healing. Medical detox programs often incorporate calming routines and meal planning to support physical recovery and help people reconnect with their basic needs.
Detox is only the first phase of recovery. While it’s intense and physically demanding, it’s also an important reset for the body and mind. Knowing what to expect—from withdrawal symptoms to organ function—can ease fears and highlight the value of medical support during this critical time.